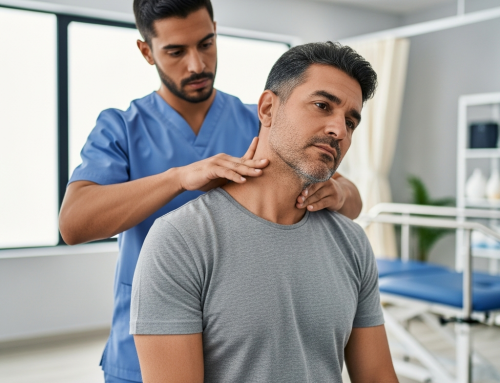
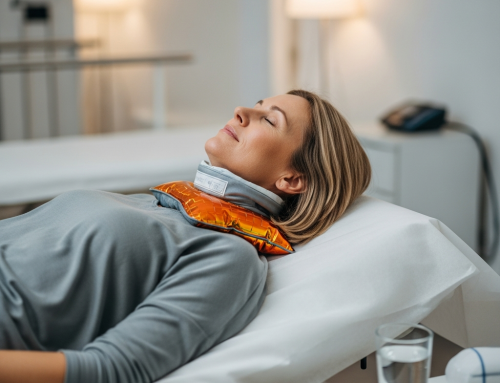
7 Symptoms of Hidden Injuries After an Auto Accident

You’re sitting at a red light, scrolling through your phone (yeah, I know you shouldn’t be), when BAM. The car behind you didn’t brake in time. Your heart pounds, your hands shake a little, but you get out and look around. No broken glass. No crumpled metal. Your neck feels… fine? Maybe a tiny bit stiff, but nothing dramatic.
“I’m okay,” you tell the other driver. “I’m okay,” you repeat to the police officer. “I’m okay,” you text your spouse.
Three days later, you wake up feeling like you got hit by a truck – which, ironically, you kind of did. Your shoulder throbs. Your back screams when you reach for your coffee mug. That headache you’ve been nursing? It’s getting worse, not better.
Welcome to the sneaky, frustrating world of hidden auto accident injuries. You know, the ones that don’t show up right away… the ones that make you question if you’re going crazy or just being dramatic.
Here’s the thing about car accidents – and I’ve seen this play out countless times with patients at our clinic. Your body is like a smartphone that’s been dropped on concrete. Sure, the screen might look fine at first glance, but sometimes the damage is happening underneath. Internal circuits get scrambled. Things stop working properly. And just like that phone, the problems don’t always show up immediately.
Why Your Body Plays Hide and Seek After an Accident
During a collision, your body floods with adrenaline faster than you can say “insurance claim.” This natural fight-or-flight response is actually pretty amazing – it masks pain, sharpens your focus, and gets you moving when you need to handle the immediate crisis. But here’s where it gets tricky: that same adrenaline can hide injuries that are absolutely real and potentially serious.
Think of adrenaline as nature’s temporary pain reliever. Except unlike the ibuprofen in your medicine cabinet, this stuff is powerful enough to make you feel invincible… temporarily. Hours or even days later, when your system finally calms down, that’s when your body starts sending you the bills for what actually happened.
And it’s not just about adrenaline. Some injuries – particularly soft tissue damage, nerve issues, and certain types of brain injuries – are like slow-developing photographs. The image becomes clearer over time, but initially? You might not see much of anything.
The Stakes Are Higher Than You Think
Look, I’m not trying to scare you, but ignoring potential hidden injuries isn’t just uncomfortable – it can derail your life in ways you haven’t even considered yet. I’ve worked with people who shrugged off “minor” accidents only to find themselves dealing with chronic pain months later. Others who developed headaches that interfered with their work performance. Some who couldn’t sleep properly for weeks because they didn’t realize they had a concussion.
The medical bills alone can be overwhelming, but there’s also lost work time, reduced quality of life, and – let’s be honest – the mental toll of wondering if you’ll ever feel “normal” again.
Plus, here’s something most people don’t think about: if you’re planning to file an insurance claim, documenting injuries early matters. A lot. Insurance companies aren’t exactly known for their generosity when you call them six months after an accident saying, “Hey, remember me? Turns out I’m hurt after all.”
What You’re About to Learn
In the next few minutes, we’re going to walk through seven symptoms that often fly under the radar after car accidents. Some might surprise you – did you know that mood changes can actually be a sign of a brain injury? Or that seemingly unrelated digestive issues might trace back to your accident?
We’ll talk about what each symptom might mean, why it happens, and – most importantly – what you should do about it. I’ll share some real stories from patients who thought they were fine… until they weren’t. And I’ll give you practical advice about when to see a doctor, what questions to ask, and how to advocate for yourself.
Because here’s what I really want you to understand: trusting your gut isn’t just good advice for dating and job interviews. It might be the most important thing you do after a car accident.
Why Your Body Plays Hide and Seek After a Crash
Here’s the thing about car accidents – your body doesn’t exactly follow the same timeline as your insurance adjuster. While they’re asking for photos and police reports within hours, your body might be sitting in the corner, quietly processing what just happened… and sometimes that processing takes days or even weeks to show up as actual symptoms.
Think of it like this: imagine someone suddenly shook a snow globe really, really hard. Sure, you can see the obvious stuff flying around immediately – the big flakes, the obvious debris. But some of those tiny particles? They settle slowly, almost invisibly, until one day you notice the whole landscape inside has shifted.
Your body works similarly after trauma. The adrenaline surge that kicks in during an accident is basically nature’s way of saying “deal with the immediate crisis first, ask questions later.” It’s incredibly effective at masking pain and injury – which makes total sense from an evolutionary standpoint. If a saber-tooth tiger was chasing our ancestors, they needed to run first and tend to their twisted ankle afterward.
The Adrenaline Masquerade
That adrenaline rush isn’t just making you feel temporarily superhuman – it’s actually changing how your nervous system processes pain signals. It’s like having a very enthusiastic but temporary personal assistant who keeps intercepting your mail. “Pain signals from the neck? Nope, we’re too busy right now. File those for later.”
This is why you might walk away from a fender-bender feeling oddly fine, even a little proud of how well you handled things… only to wake up three days later feeling like you’ve been used as a punching bag. Your body wasn’t lying to you initially – it was just prioritizing survival over a full damage assessment.
When Soft Tissues Tell Their Story
Now, here’s where things get particularly tricky. Unlike broken bones, which show up pretty dramatically on X-rays (hard to miss a crack in a femur), soft tissue injuries are more like… well, imagine trying to photograph a bruise on the inside of a peach. The damage is real, but it’s not always immediately visible, even to medical professionals.
Soft tissues – your muscles, ligaments, tendons, and the fascia that wraps around everything like biological plastic wrap – can stretch, tear, or inflame in ways that don’t announce themselves right away. A muscle might develop micro-tears that only start screaming when the initial shock wears off and normal movement resumes.
The Delayed Reaction Club
This delayed onset is so common it has its own medical terminology. Healthcare providers actually expect certain symptoms to appear 24-72 hours post-accident. It’s not that you’re being dramatic or that something new is wrong – it’s that your body is finally getting around to filing those incident reports that got backlogged during the initial emergency response.
Think about how you might feel the day after an unusually intense workout. You probably felt pretty good right afterward – endorphins pumping, sense of accomplishment, maybe even energized. But the next morning? That’s when your muscles send their strongly worded complaint letters about what you put them through.
Car accidents create a similar scenario, except instead of voluntarily doing too many squats, your body got subjected to forces it definitely didn’t sign up for.
The Invisible Nature of Many Injuries
Here’s what’s particularly frustrating about post-accident injuries: some of the most debilitating ones are also the most invisible. A concussion doesn’t show up as dramatically as a cast on your leg. Whiplash doesn’t announce itself with obvious swelling. Nerve irritation might not have any external signs at all.
This invisibility can be emotionally challenging too. When people can’t see your injury, there’s sometimes an unspoken assumption that it’s not “real” or significant. But anyone who’s dealt with chronic pain, headaches, or cognitive fog after an accident knows these hidden injuries can be just as – if not more – disruptive than obvious ones.
The key thing to remember? Your body doesn’t follow anyone else’s timeline for recovery, and symptoms that appear days or weeks later aren’t necessarily “new” problems. They’re often just your body’s way of finally getting your attention about damage that happened during those chaotic moments when everything else took priority.
When to Actually Worry (And When to Relax)
Here’s the thing about post-accident symptoms – they don’t follow a neat timeline. You might feel perfectly fine for three days, then wake up on Thursday morning feeling like you wrestled a bear. That’s… actually pretty normal.
But some red flags deserve immediate attention. If you’re experiencing severe headaches that get worse over time, confusion, repeated vomiting, or any numbness that spreads, don’t wait. We’re talking emergency room territory here. Same goes for chest pain that doesn’t ease up or difficulty breathing that feels different from normal anxiety.
The tricky part? Distinguishing between “I’m sore because my body got jerked around” and “something’s actually wrong.” When in doubt, document everything. Take photos of bruises as they develop – they often get worse before they get better. Keep a simple pain journal on your phone, rating discomfort from 1-10 throughout the day.
The 48-72 Hour Rule (That Nobody Tells You About)
Most doctors won’t mention this, but there’s a sweet spot for seeking treatment after an accident. The first 48-72 hours are crucial for soft tissue injuries. Your body’s initial shock response can mask pain, but once that adrenaline wears off… well, that’s when you really feel what happened.
Don’t wait for pain to become unbearable. Actually, here’s a secret from the treatment side – patients who come in during this window typically respond better to therapy. Your tissues are still in that acute phase where they’re more receptive to gentle intervention.
Ice is your friend for the first 48 hours (20 minutes on, 40 minutes off), but after that? Switch to heat. And please, resist the urge to “push through” neck stiffness or back pain. You’re not being tough – you’re potentially making things worse.
Documentation That Actually Matters
Forget fancy apps or complicated tracking systems. Here’s what insurance companies and doctors actually want to see
Daily photos of visible injuries, even if they seem minor. Bruising patterns can reveal impact points that help medical professionals understand what happened to your body. Take them in good lighting, preferably natural light near a window.
Sleep disruption notes. Can’t fall asleep? Waking up at 3 AM? Write it down. Sleep problems after accidents are incredibly common and often indicate underlying issues that need addressing.
Activity limitations. Be specific – “can’t turn head fully to the right when backing out of driveway” is way more useful than “neck hurts.”
One thing that surprises people… keep receipts for everything accident-related. That heating pad you bought? The extra pillows for better sleep positioning? Even Uber rides to medical appointments. These little expenses add up, and they’re often reimbursable.
The Treatment Shopping Game Plan
Not all healthcare providers understand auto accident injuries equally well. Your family doctor might be amazing for annual checkups but completely stumped by whiplash mechanics.
Start with providers who specialize in accident care – physical medicine doctors, chiropractors who work with personal injury cases, or physical therapists experienced with motor vehicle accidents. They speak the insurance language and understand documentation requirements.
But here’s something I wish more people knew… you don’t have to stick with the first provider you see. If someone dismisses your symptoms or seems rushed, find someone else. Your accident case allows you to be picky about providers – use that flexibility.
The Insurance Maze (Simplified)
Insurance companies bank on people not understanding their coverage. Here’s your cheat sheet
Personal Injury Protection (PIP) typically covers initial medical expenses regardless of fault. Use it. Don’t let it sit there while you suffer.
Document every conversation with insurance adjusters. Get claim numbers, representative names, reference numbers for calls. Send follow-up emails confirming what was discussed.
The biggest mistake? Giving recorded statements before talking to anyone knowledgeable about your rights. Those friendly adjusters asking “how are you feeling?” aren’t just being nice – they’re gathering information that might limit your claim later.
And that quick settlement offer that seems generous? It probably isn’t. Most hidden injuries don’t fully reveal themselves for weeks or even months. Don’t rush into agreements when you don’t know the full scope of your situation yet.
Remember – you’ve got one body, and it needs to last you a long time. Taking care of it properly now isn’t being dramatic… it’s being smart.
When Your Body Whispers Instead of Screams
Here’s what nobody tells you about hidden injuries – they’re sneaky little troublemakers that mess with your head as much as your body. You’ll find yourself second-guessing everything. “Is this real pain, or am I just being dramatic?” (Spoiler alert: if you’re asking that question, it’s probably real.)
The biggest challenge? Most people expect injury pain to announce itself like a fire alarm. Instead, hidden injuries are more like that annoying drip in your kitchen sink – barely noticeable at first, then suddenly it’s driving you absolutely crazy at 2 AM.
The “I Feel Fine” Trap
Right after an accident, your body floods with adrenaline. You’re basically running on nature’s own energy drink… which means you might feel invincible for hours, even days. Then reality crashes in like an unwelcome house guest.
This creates a perfect storm of doubt. You told everyone you were fine. Your insurance company has it on record. Your boss expects you back at work tomorrow. Now you’re dealing with neck pain that feels like someone’s slowly tightening a vice, and you’re wondering if people will think you’re making it up.
Solution: Document everything from day one, even if you feel okay. Take photos of any marks, bruises, or swelling – no matter how minor. Keep a simple pain diary on your phone. Just quick notes: “Day 2 – stiff neck when turning left” or “Day 5 – headache behind right eye, lasted 3 hours.”
This isn’t paranoia; it’s protection. For your health and your legal standing.
The Insurance Company Dance
Let’s be real about insurance companies – they’re not exactly known for their generosity. They have one job: pay out as little as possible while staying within legal boundaries. When you have hidden injuries, you’re fighting an uphill battle because the evidence isn’t screaming at them.
You’ll get asked the same questions repeatedly. You might feel like they’re trying to catch you in some kind of contradiction. They are. It’s nothing personal – it’s just business to them.
Solution: Get medical attention within 72 hours of your accident, regardless of how you feel. Yes, even if you think it’s unnecessary. Here’s why – many insurance policies require prompt medical attention, and waiting weeks to see a doctor gives them ammunition to argue your injuries aren’t accident-related.
Find a healthcare provider experienced with auto accident injuries. They understand the delayed onset patterns and know how to document findings properly. Your family doctor might miss subtle signs that a specialist would catch immediately.
The Employer Expectations Game
This one’s particularly tricky if you have a physical job or if your workplace isn’t exactly… understanding about medical issues. You might feel pressure to “tough it out” or worry about job security if you need accommodations.
Some employers act like requesting modified duties is asking for the moon, when really you just need to avoid lifting heavy boxes for a few weeks while your back heals.
Solution: Be proactive with communication. Don’t wait until you’re struggling to have the conversation. Approach your supervisor with potential solutions, not just problems. “I’m dealing with some residual effects from my accident, but I’ve spoken with my doctor about modifications that would keep me productive while I recover.”
Get workplace accommodations in writing – even something as simple as an email confirming adjusted duties. This protects you if symptoms worsen or if there’s confusion later about what was agreed upon.
When Family and Friends Don’t Get It
This might be the hardest part. People who care about you might not understand why you’re “still complaining” about an accident that happened weeks ago. They can see you walking around, talking normally… you look fine to them.
Comments like “At least it wasn’t worse” or “Maybe you just need to get back to your routine” come from a good place, but they sting when you’re genuinely struggling.
Solution: Help them understand without becoming a broken record. Share specific information: “The doctor explained that soft tissue injuries often take 6-12 weeks to heal completely” rather than just saying “I’m still hurting.”
Set boundaries around the topic if needed. You don’t owe anyone a detailed explanation of your symptoms every day. A simple “I’m following my doctor’s treatment plan and taking it day by day” can redirect well-meaning but unhelpful conversations.
Remember – healing isn’t linear, and hidden injuries are still real injuries. Trust your body, advocate for yourself, and don’t let anyone rush your recovery process.
What to Expect in the Days and Weeks Ahead
Here’s the thing about hidden injuries – they’re sneaky little troublemakers that don’t follow our preferred timeline. You might feel completely fine today and wake up tomorrow wondering if a truck ran over you in your sleep. Or maybe you’re already feeling some discomfort and wondering… is this going to get worse?
The honest truth? The first 24-72 hours are often the most telling. Your body’s still running on adrenaline right after an accident, masking pain signals like a really effective but temporary painkiller. As that wears off, inflammation sets in, muscles start to tighten, and your nervous system begins to actually process what happened.
Don’t panic if you feel worse on day two or three than you did right after the accident. That’s actually pretty normal – frustrating, but normal. Your body’s just… catching up to reality.
The Two-Week Mark – When Things Usually Reveal Themselves
Most hidden injuries start showing their true colors within the first two weeks. Soft tissue injuries like whiplash typically peak around day 2-5, then gradually improve over the following weeks. But – and this is important – some symptoms can take longer to surface.
Concussion symptoms, for instance, can be especially tricky. You might feel fine for a few days, then suddenly find yourself struggling with concentration or feeling unusually emotional. That’s your brain saying, “Hey, remember that jarring we experienced? Yeah, I’m still processing that.”
If you’re dealing with back or neck pain, expect some ups and downs. Good days followed by rough ones. It’s like your body’s playing a game of “will it hurt today or won’t it?” – not exactly fun, but totally within the realm of normal healing.
When Professional Help Makes Sense
Look, I get it. Nobody wants to be “that person” who makes a big deal out of everything. But here’s what I’ve learned from watching countless people navigate post-accident recovery: waiting too long to address symptoms usually makes things take longer to resolve, not shorter.
Consider seeing a healthcare provider if you’re experiencing any persistent symptoms beyond the first few days. And by persistent, I mean anything that’s not clearly improving or is interfering with your daily life. Having trouble sleeping because your neck aches? That counts. Headaches that won’t quit? Definitely worth checking out.
Don’t wait for pain to become unbearable – that’s like waiting for a small leak to flood your basement before calling a plumber. Early intervention often means faster, more complete recovery.
Documentation – Yes, It Matters
I know paperwork is about as exciting as watching paint dry, but keeping track of your symptoms can be incredibly valuable. Not just for insurance purposes (though that matters too), but for your own understanding of what’s happening.
Jot down how you’re feeling each day – even just a quick note on your phone. “Woke up with stiff neck, felt better after lunch, headache around 3 PM.” Simple stuff, but it helps identify patterns and shows healthcare providers what’s really going on.
Photos of any visible injuries, even minor ones, can also be helpful down the road. Bruising often gets worse before it gets better, and what looks like nothing today might tell a different story tomorrow.
Recovery Isn’t Always Linear (And That’s Okay)
Here’s something they don’t always tell you – healing isn’t a straight line from “hurt” to “completely fine.” You’ll have good days that make you think you’re all better, followed by setbacks that make you wonder if you’re ever going to feel normal again.
That roller coaster? Completely normal. Your body’s working hard to repair itself, and sometimes that means taking a step back before moving forward again. Be patient with yourself… easier said than done, I know.
Most people with minor to moderate accident-related injuries see significant improvement within 6-12 weeks. But everyone’s different – your age, overall health, the specifics of your accident, and how quickly you address symptoms all play a role in your recovery timeline.
Moving Forward with Confidence
The bottom line is this: trust your body, but don’t ignore warning signs. You know yourself better than anyone, and if something feels off, it probably is. Getting checked out doesn’t make you weak or dramatic – it makes you smart.
Take care of yourself the same way you’d take care of someone you love who’d been through the same experience. With patience, attention, and the understanding that healing takes time.
Look, I get it – after a car accident, the last thing you want to think about is whether something might be wrong when you’re already dealing with insurance calls, car repairs, and a million other headaches. It’s so much easier to tell yourself you’re fine and push through. That’s just human nature.
But here’s the thing… your body has this incredible way of protecting you in the moment. Adrenaline kicks in, shock takes over, and you might not feel the full impact – literally and figuratively – until days or even weeks later. That stiff neck you’ve been ignoring? Those headaches that seem to come out of nowhere? The way you’ve been feeling just a little “off” lately? They’re not necessarily normal parts of getting older or stress from everything else going on.
Think of it like this – your body is basically sending you text messages, and some of them are really important. The challenge is knowing which ones need your immediate attention versus the ones that can wait. And honestly? When it comes to injuries from accidents, it’s better to check in with someone who can help you decode those messages properly.
I’ve seen too many people – smart, capable people just like you – who waited months before addressing symptoms that could have been treated much more easily if caught early. Not to scare you, but some of these hidden injuries? They have a way of becoming not-so-hidden if left alone too long. Your neck, your back, your nervous system – they’re all pretty complex systems that sometimes need a little professional TLC to get back on track.
The good news is that you don’t have to figure this out alone. Whether it’s persistent pain, cognitive issues, sleep problems, or just that nagging feeling that something isn’t quite right, there are people who specialize in exactly this kind of thing. And no, you’re not being dramatic or weak for seeking help – you’re being smart.
Medical professionals who work with accident-related injuries see these patterns all the time. They know what to look for, which symptoms tend to cluster together, and most importantly, how to help you feel like yourself again. Sometimes it’s physical therapy, sometimes it’s addressing inflammation you didn’t even know you had, sometimes it’s just having someone validate that yes, what you’re experiencing is real and treatable.
Your health isn’t something to gamble with, especially when help is available. If any of these symptoms sound familiar – or if you’ve got that gut feeling that something just isn’t right – consider reaching out to someone who can give you proper answers. You deserve to feel good in your own body again.
Ready to get some clarity about how you’re really doing after your accident? Our team understands exactly what you’re going through, and we’re here to help you sort through what’s normal healing versus what might need attention. Give us a call – sometimes just talking through your symptoms with someone who gets it can be the first step toward feeling like yourself again.