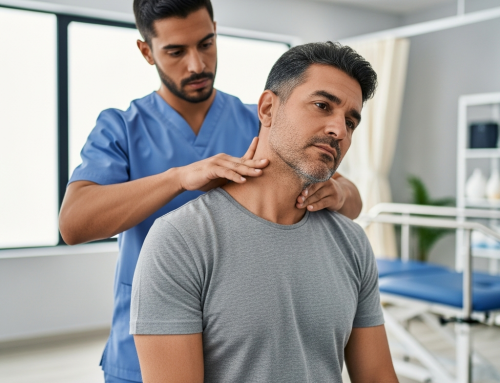
9 Ways Early Treatment Improves Auto Accident Recovery
You’re sitting at a red light, scrolling through your phone for just a second – we’ve all been there – when BAM. The world jolts forward, your coffee flies everywhere, and suddenly you’re dealing with that awful mix of adrenaline and confusion that comes with being rear-ended.
In those first few moments, you’re probably thinking about your car, the other driver, maybe calling your insurance company. What you’re probably NOT thinking about? How the next few hours and days could completely change your recovery trajectory.
Here’s the thing that most people don’t realize until it’s too late: those first 72 hours after an auto accident are absolutely critical. Not just for the legal stuff or getting your car towed, but for your body’s ability to heal properly. I’ve seen it countless times in our clinic – two people with nearly identical injuries, but one sought treatment immediately while the other waited “to see if it would get better on its own.” Guess who’s still dealing with chronic pain six months later?
Your body is basically a really sophisticated alarm system, and when trauma hits – even what seems like a “minor” fender bender – everything goes into high alert mode. Inflammation kicks in, muscles tense up to protect potentially injured areas, and your nervous system starts firing warning signals left and right. This is actually good… initially. But when these protective mechanisms stay activated for weeks or months because they weren’t properly addressed early on? That’s when short-term injuries transform into long-term problems.
Think of it like a small leak in your roof. You could ignore it, hope it stops raining, maybe put a bucket underneath. But that small leak? It’s going to cause way more damage over time than if you’d just fixed it right away. Your body works the same way after trauma.
The frustrating part is that you might feel “fine” initially. Adrenaline is an incredible painkiller – nature’s way of helping you handle emergencies. But as that wears off over the next day or two, that’s when the real picture starts to emerge. Suddenly your neck feels stiff, your back aches in ways it never has before, maybe you’re getting headaches or feeling more tired than usual.
And here’s what really gets me fired up about this topic: the medical system often fails people after auto accidents. You go to the ER, they make sure nothing’s broken or bleeding, maybe give you some pain meds, and send you home with advice to “rest and follow up with your doctor if symptoms persist.” That’s like telling someone with a sprained ankle to just walk it off and come back if it’s still hurting next month.
What if I told you there were specific things you could do – starting immediately after an accident – that could cut your recovery time in half? Or prevent those nagging symptoms from turning into chronic conditions that affect your sleep, work, and quality of life for months or even years?
I’m not talking about anything complicated or expensive here. These aren’t secrets that only doctors know, or treatments that require special equipment. They’re practical, evidence-based approaches that address how your body actually responds to trauma. Some of them might surprise you – like why certain types of gentle movement in the first few days can be more effective than complete rest, or how specific timing around inflammation can make or break your healing process.
The reality is that early intervention isn’t just about feeling better faster (though that’s certainly nice). It’s about preventing your body from developing compensatory patterns that can create problems in completely different areas months down the road. It’s about keeping acute injuries from becoming chronic pain conditions. It’s about getting back to your normal life instead of adjusting to a “new normal” that includes daily discomfort.
Whether you were just in an accident yesterday or you’re reading this “just in case” – because let’s face it, none of us plans to get hit by a distracted driver – what you’re about to learn could save you months of unnecessary pain and frustration. We’re going to walk through nine specific strategies that can dramatically improve your recovery, and more importantly, why each one works the way it does.
Because knowledge is power, especially when it comes to your health.
What Actually Happens When Your Body Gets Banged Up
Think of your body like a really well-orchestrated symphony – everything’s humming along beautifully until suddenly, BAM. A car accident is like someone throwing a wrench right into the middle of that orchestra. The musicians (your muscles, joints, and tissues) don’t just stop playing… they start playing completely different, chaotic songs.
Here’s what’s wild though – and this might surprise you – a lot of the damage from car accidents isn’t actually from the initial impact. It’s from what happens in the hours and days afterward when your body tries to “fix” things on its own.
Your body’s immediate response is basically to throw everything into lockdown mode. Muscles tense up like they’re bracing for another hit that’s never coming. Inflammation floods the area like an overzealous security team that won’t stand down even after the threat’s gone. And your nervous system? It’s basically hitting the panic button on repeat.
The Sneaky Truth About Adrenaline
You know that surge you feel right after an accident where you’re like “I’m totally fine!” and you’re walking around, talking to police officers, maybe even declining the ambulance? Yeah, that’s adrenaline doing what it does best – masking pain and making you feel invincible.
It’s kind of like when you’re cleaning house before guests arrive and you suddenly have superhuman energy to move furniture and scrub baseboards. Except in this case, your body’s pumping you full of natural painkillers and stress hormones that can hide serious injuries for hours, sometimes even days.
I’ve seen people who felt perfectly normal at the scene of an accident, went home, slept it off… and then woke up feeling like they’d been hit by a truck. Again. Because in a way, they had been.
Why “Wait and See” Usually Backfires
Here’s where things get counterintuitive. Most of us are raised with this idea that the body heals itself, right? Rest, ice, maybe some ibuprofen, and you’ll be good as new. And honestly, for a lot of minor injuries, that’s totally true.
But car accidents create what doctors call “complex trauma patterns” – which is a fancy way of saying your body gets confused about what to fix first and how to fix it. It’s like trying to renovate a house while you’re still living in it and half the rooms are flooded.
Your muscles might start compensating for an injured joint by working overtime, which then creates tension in completely different areas. Your neck might stiffen up to protect a sore spot, which throws off your shoulder blade, which messes with your lower back… you get the idea. It’s this whole cascade effect that can turn a relatively minor injury into a months-long ordeal.
The Inflammation Trap
Now, inflammation gets a bad rap these days, but it’s actually your body trying to help. Think of it like your internal emergency response team rushing to the scene with supplies and equipment. The problem is, sometimes they set up camp and just… never leave.
In the first few hours after an accident, inflammation is doing important work – bringing healing nutrients to injured tissues, clearing out damaged cells, starting the repair process. But if it hangs around too long (which it often does without proper treatment), it starts causing more problems than it solves.
It’s like having house guests who come to help you move but then decide to stick around for three months. What started as helpful becomes… not so helpful.
Your Body’s Memory Bank
Here’s something that sounds almost too weird to be true – your body actually “remembers” trauma. Not just emotionally (though that’s real too), but physically. Your muscles, fascia, and nervous system can hold onto tension patterns long after the initial injury has healed.
It’s similar to how you might unconsciously tense up when driving past the intersection where your accident happened, except your shoulder muscles might be doing the same thing every time you turn your head a certain way.
This is why some people develop chronic pain or stiffness months after what seemed like a minor fender-bender. Their body essentially got stuck in “protection mode” and forgot how to relax back into normal patterns.
The good news? Early intervention can essentially help your body “unlearn” these protective patterns before they become your new normal.
Start Moving (But Not Like You Think)
Here’s what most people get wrong about post-accident movement – they either become couch potatoes or weekend warriors. Both are mistakes.
Your body needs gentle, purposeful movement within the first 48 hours. I’m talking about slow neck rotations while you’re watching TV, ankle pumps during commercial breaks, and yes… walking to the mailbox counts. The key word here is gentle. You’re not training for a marathon – you’re keeping your joints from turning into rusty hinges.
But here’s the insider tip: set phone alarms every two hours during your waking hours. When it goes off, do something. Stand up. Roll your shoulders. Take five deep breaths. Your future self will thank you when you’re not moving like the Tin Man three days later.
The 72-Hour Documentation Rule
Most people think documentation means taking a few photos and calling it good. That’s… not enough.
Start a voice memo app on your phone right now. Every morning for the first week, record how you feel. “Day three after the accident. Left shoulder still aches when I reach for coffee. Headache is about a 4 out of 10.” This isn’t being dramatic – it’s being smart.
Why? Because three weeks from now, when you’re sitting across from an insurance adjuster or healthcare provider, you won’t remember if your headache started on day two or day five. But your phone will. Take photos of any visible injuries every other day, even if they seem minor. Bruises have this sneaky way of getting worse before they get better.
And here’s something nobody tells you – keep receipts for everything. That extra pillow for neck support? Receipt. The heating pad? Receipt. Even the Epsom salts. These add up, and they’re all part of your recovery costs.
Find Your Treatment Team (Before You Need Them)
Don’t wait until you’re in serious pain to start researching healthcare providers. When you’re hurting, you’ll grab the first available appointment – which might not be the right fit.
Start with your primary care doctor, but also research local physical therapists, chiropractors, and massage therapists who specialize in auto accident injuries. Read their Google reviews, but pay attention to the negative ones too. Do people complain about wait times? Billing issues? Dismissive attitudes? Those are red flags.
Here’s a pro tip: call their offices and ask about their experience with auto accident cases. Some providers get nervous about insurance claims and might be reluctant to take you on. You want someone who’s comfortable with the process and won’t drop you if things get complicated.
The Insurance Game Plan
Insurance companies aren’t your enemy, but they’re definitely not your best friend either. They have one job: minimize payouts. Understanding this changes everything about how you approach them.
First rule: be honest but don’t downplay your symptoms. If your neck hurts, say your neck hurts. Don’t say “it’s probably nothing” or “I’m sure it’ll get better soon.” These statements can come back to haunt you later.
Second rule: get everything in writing. That friendly adjuster who promises to “take care of everything”? Nice, but not legally binding. Follow up phone conversations with emails summarizing what was discussed.
And here’s something most people don’t know – you have the right to choose your own healthcare providers in most states. The insurance company might suggest their “preferred providers,” but you’re not required to use them. Sometimes these preferred providers are excellent… sometimes they’re just cheap.
Know When to Escalate
The biggest mistake people make? Assuming they’ll “just get better” and waiting too long to seek help.
Your body has an amazing ability to compensate for injuries. That slightly sore neck might not seem like a big deal now, but three months later when you’ve developed chronic tension headaches because your neck muscles have been overcompensating… well, that’s a much bigger problem.
Watch for these red flags: pain that’s getting worse instead of better after a week, numbness or tingling anywhere, persistent headaches, or sleep disruption that goes beyond a few restless nights.
Don’t be a hero. Early intervention almost always leads to better outcomes and – honestly – lower total costs. That $200 physical therapy session now might save you from $2,000 worth of treatment later.
When Your Body Feels Like It’s Betraying You
Let’s be honest – the first few weeks after an accident can feel absolutely awful. You wake up stiff as a board, your neck screams when you turn your head, and that “minor” back twinge has somehow turned into a constant companion. Here’s what really happens: your body goes into protective mode, and sometimes… it gets a little too enthusiastic about the whole protection thing.
Your muscles tense up like they’re preparing for another impact that’s never coming. It’s exhausting, frankly. And then there’s the guilt – you look fine on the outside, so why does everything hurt so much?
The solution isn’t just “rest and ice” (though both have their place). Early treatment works because it interrupts this protective cycle before it becomes your new normal. Physical therapy, for instance, teaches your nervous system that it’s safe to move again. That gentle manipulation and targeted exercises? They’re essentially having a conversation with your body, saying “Hey, we’re okay now. You can relax.”
The Insurance Maze – Because Paperwork Never Sleeps
Oh, insurance companies. They’re like that friend who’s helpful… eventually… after you’ve jumped through seventeen hoops and provided documentation for things you didn’t even know existed.
Here’s what trips most people up: they assume their regular health insurance will cover accident-related injuries the same way it covers, say, a broken arm from skiing. Plot twist – it often doesn’t work that way. Auto insurance (yours or the other driver’s) typically needs to be the primary payer, but getting that sorted out can take weeks. Meanwhile, you’re sitting there in pain, afraid to seek treatment because you don’t know what it’ll cost.
The trick? Don’t wait. Many healthcare providers who specialize in auto accidents will work with you on payment arrangements or accept what’s called a “letter of protection” – basically a promise that they’ll get paid once your insurance claim settles. It’s not charity; it’s smart business on their part because early treatment often leads to better outcomes and lower overall costs.
Also – and this is important – document everything. Every ache, every sleepless night, every time you can’t turn your head to check your blind spot. Insurance companies love to minimize injuries that aren’t immediately visible on an X-ray.
When “Just Push Through It” Becomes Your Worst Enemy
We live in a culture that celebrates toughing it out. Walked it off. Powered through. And sometimes… that mentality can really mess with your recovery.
I’ve seen too many people who ignored early warning signs because they didn’t want to seem weak or dramatic. They convinced themselves that the headaches would go away, that the shoulder pain was just stress, that sleeping poorly was normal after a traumatic event. Months later, they’re dealing with chronic issues that could have been prevented with early intervention.
Your pain isn’t a character flaw. It’s information. And honestly? Ignoring it doesn’t make you tough – it just makes recovery harder down the road.
The solution starts with changing your mindset. Think of early treatment like changing the oil in your car – it’s maintenance, not weakness. You wouldn’t drive 20,000 miles on old oil and then act surprised when your engine seizes up, right?
The Mental Game Nobody Warns You About
Here’s something they don’t tell you in those insurance pamphlets: accidents mess with your head in ways that have nothing to do with whether you hit your skull.
Suddenly, you’re hyperaware of every car around you. That intersection where it happened? Your heart races every time you approach it. You might find yourself gripping the steering wheel tighter, checking your mirrors obsessively, or just feeling… off. Some people develop what feels like a general anxiety they can’t quite place.
This isn’t uncommon, and it’s not “all in your head” in the dismissive way people sometimes mean. Your nervous system took a hit, and it’s trying to protect you from future threats – even imaginary ones.
The fix often involves treating both the physical and emotional aspects of trauma simultaneously. Many progressive treatment centers now integrate counseling or stress management techniques with traditional physical therapy. Because here’s the thing – your brain and body aren’t separate entities. They’re having a constant conversation, and after an accident, that conversation can get pretty chaotic.
Sometimes the best thing you can do is acknowledge that recovery isn’t linear. Some days will be better than others, and that’s completely normal.
What to Expect in Those First Few Weeks
Let’s be honest – you’re probably wondering when you’ll feel “normal” again. And that’s completely understandable, especially when your body feels like it belongs to someone else right now.
Here’s the thing about auto accident recovery: it’s rarely linear. You might have a good day where you think “Great! I’m getting better!” followed by a rough patch that makes you wonder if you’re moving backwards. That’s not failure – that’s normal healing.
Most people see initial improvements within the first 2-4 weeks of starting treatment, but – and this is important – improvement doesn’t mean you’re done. Think of it like learning to play piano… you don’t go from choppy scales to Mozart overnight. Your body needs time to rebuild strength, restore proper movement patterns, and calm down that overprotective nervous system.
Pain levels typically start decreasing around week 3-6, though some days will still be harder than others. Sleep usually improves first (thank goodness), then daily activities start feeling less daunting. The stuff that takes longest? Complex movements, heavy lifting, those activities that require your whole body working in perfect harmony.
When Your Body Keeps Score
Your body remembers trauma – not just emotionally, but physically. That tension you’re holding in your shoulders? The way you’re moving differently than before? Your nervous system is basically saying “Hey, let’s be extra careful here.”
This protective mode is helpful initially, but it can overstay its welcome. Early treatment helps teach your body that it’s safe to move again, to trust itself. Without this guidance, some people develop compensation patterns that stick around long after the original injury heals.
You might notice muscle spasms, headaches, or stiffness that seems to migrate around your body. This isn’t your imagination – it’s your body trying to protect areas that don’t actually need protecting anymore. Professional treatment helps sort out what needs attention versus what needs reassurance.
Creating Your Recovery Roadmap
Most comprehensive recovery plans unfold in phases. Initially, we’re focused on pain management and restoring basic function – getting you through daily activities without wincing. This usually takes 4-8 weeks, depending on your injuries.
Phase two is where things get interesting. We start addressing those deeper movement patterns, building strength, and tackling the activities that matter to you. Maybe it’s picking up your toddler without hesitation, or getting back to your weekend hiking routine. This phase can last 2-4 months… sometimes longer for more complex cases.
The final phase? That’s about bulletproofing your recovery. Building resilience so your body can handle life’s curveballs – whether that’s a long day of yard work or another fender bender down the road.
Red Flags vs. Normal Healing Drama
Sometimes symptoms get worse before they get better, especially in those first few weeks of treatment. Your body might be like “Wait, we’re moving again? I wasn’t prepared for this!”
But there are some warning signs that shouldn’t be ignored. Increasing neurological symptoms – numbness, tingling, weakness that’s getting worse rather than better – need immediate attention. Severe headaches that aren’t responding to treatment, dizziness that’s interfering with basic activities, or pain that’s becoming more intense rather than gradually improving… these warrant a conversation with your healthcare team.
Normal healing drama includes some good days and bad days, temporary flare-ups after doing too much too soon, and that general feeling of “I’m better but not quite right yet.” Your body is literally rebuilding itself – give it some grace.
The Long Game
Here’s what nobody tells you about auto accident recovery: it’s not just about getting back to where you were. It’s often an opportunity to build better movement patterns, address weaknesses you didn’t know existed, and develop a deeper understanding of how your body works.
Many of our patients actually end up stronger and more resilient than before their accident. Not because getting hurt was good for them – nobody wants that – but because the recovery process taught them things about their bodies they never knew.
The timeline isn’t everything, though I know you want concrete answers. Focus on the trend rather than daily fluctuations. Are you sleeping a bit better this week than last? Can you turn your neck a little further? These small victories add up to something significant.
Recovery isn’t about racing back to your old life – it’s about building a better foundation for whatever comes next.
Your Recovery Doesn’t Have to Be Perfect – It Just Has to Be Yours
Here’s what I want you to know… and this comes from watching countless people navigate their healing after accidents: there’s no such thing as the “right” way to recover. Some folks bounce back in weeks, others take months, and that’s completely normal. Your body – and your mind – will heal at their own pace.
But here’s the thing that really matters: when you start matters more than how fast you finish.
Those nine strategies we’ve talked about? They’re not just medical recommendations written on some chart. They’re your toolkit for taking back control when everything feels uncertain. Early physical therapy sessions that seem small today can prevent months of chronic pain tomorrow. That initial mental health check-in might feel unnecessary now, but it’s actually you being incredibly smart about your long-term wellbeing.
I’ve seen people wait – thinking they’re being tough, hoping things will just… resolve themselves. And sometimes they do. But more often? Those little aches turn into bigger problems. That anxiety about driving again becomes a years-long struggle. The insurance paperwork that seemed manageable suddenly feels overwhelming.
You don’t have to be that person.
Think of early treatment like tending to a garden after a storm. Sure, some plants might naturally recover on their own. But the ones you water, support with stakes, and give extra attention? Those are the ones that come back stronger than before. That’s what we’re talking about here – not just getting back to where you were, but potentially ending up in an even better place.
The beautiful thing about starting early is that it gives you options. More treatment choices. Better outcomes. Time to explore what works best for your specific situation. It’s like having a longer runway when you’re trying to take off – everything becomes more possible.
And look, I get it. Maybe you’re reading this thinking, “But I feel okay right now…” or “I don’t want to make a big deal out of this.” Those feelings are valid. But feeling okay today and preventing problems down the road? Those aren’t mutually exclusive things.
You’re Not Meant to Figure This Out Alone
Recovery isn’t a solo sport, even though it sometimes feels that way. Whether you’re dealing with lingering pain, struggling with the emotional aftermath, or just feeling overwhelmed by all the moving pieces – reaching out isn’t admitting defeat. It’s being smart.
Our team understands that every accident is different, every person is different, and every recovery looks different. We’re not here to rush you or pressure you into anything. We’re here to listen, to understand what you’re experiencing, and to help you explore your options.
If something we’ve discussed resonates with you, or if you’re just not sure what your next step should be, give us a call. Sometimes the most helpful conversation starts with, “I’m not even sure what questions to ask…” And that’s perfectly okay. We’ll figure it out together.
Your recovery matters. You matter. And you don’t have to navigate this path alone.