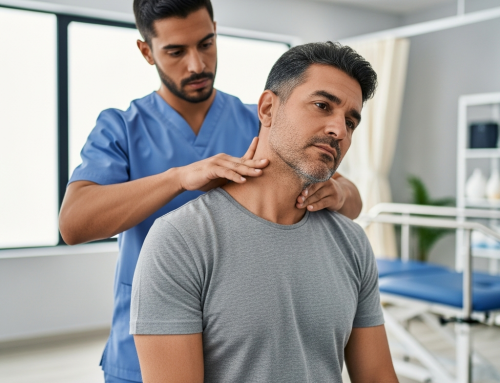
10 FAQs About Car Accident Treatment
The moment it happens, everything changes.
One second you’re thinking about dinner plans or that meeting tomorrow, and the next? You’re sitting in your car – maybe it’s steaming, maybe there’s broken glass, maybe you’re just stunned – wondering what the hell just happened. Your heart’s pounding, your hands are shaking, and somewhere in the back of your mind, this little voice is asking: “Am I hurt? Should I feel worse than I do right now?”
Here’s the thing about car accidents – they’re sneaky. Not just the accidents themselves (though, yeah, nobody plans to get rear-ended at a red light), but the way your body responds afterward. You might walk away feeling perfectly fine, even a little proud of how well you handled everything. You exchange insurance information like a responsible adult, maybe even crack a joke with the other driver. “Well, that could’ve been worse, right?”
Then you wake up the next morning feeling like you’ve been hit by a truck. Which… technically, you were.
This is where things get complicated. Because now you’re dealing with insurance companies who want to close your case yesterday, doctors who might not understand the connection between that “minor fender bender” and your sudden neck pain, and well-meaning friends who keep saying, “At least it wasn’t serious.” Meanwhile, you’re popping ibuprofen like candy and wondering if you should’ve gone to the ER immediately instead of driving yourself home.
Sound familiar? You’re not alone. Every year, millions of people find themselves in this exact situation – caught between what they think they should feel after a car accident and what their body is actually telling them. The problem is, most of us know more about our car insurance coverage than we do about how to handle the medical side of things after an accident.
And that’s… well, that’s a problem. Because here’s what nobody tells you: how you handle your medical care in those first few weeks after an accident can literally change the trajectory of your recovery. Get it right, and you might bounce back without any lasting issues. Get it wrong – or worse, ignore it completely – and you could be dealing with chronic pain, mobility issues, and a mountain of medical bills for years to come.
I’ve seen it happen too many times. People who shrug off that initial soreness, thinking it’ll just go away on its own. People who accept the first doctor’s opinion without question, even when something doesn’t feel right. People who let their insurance company call the shots about their treatment because, honestly, they don’t know what questions to ask.
The truth is, navigating medical care after a car accident feels like learning a foreign language while you’ve got a headache. There are terms you’ve never heard before, procedures you don’t understand, and everyone seems to be speaking in acronyms. PIP coverage, MRI protocols, treatment modalities – it’s enough to make your head spin (and it might already be spinning from the accident).
That’s exactly why we put together this guide. Not because we love talking about car accidents – trust me, we’d rather everyone stay safe on the roads. But because when accidents do happen, we want you to be prepared. We want you to know what questions to ask, what red flags to watch for, and how to advocate for yourself when you’re feeling vulnerable.
Over the next few minutes, we’re going to walk through the ten questions we hear most often from people who’ve been in car accidents. Things like whether you should see a doctor even if you feel fine (spoiler alert: probably), how to know if your symptoms are “normal” or something to worry about, and what to do when your insurance company starts pressuring you to settle before you’ve fully recovered.
We’ll talk about why some doctors understand accident injuries better than others, how to document everything properly (because yes, that matters more than you think), and what treatment options actually work versus the ones that just eat up your time and money.
Most importantly? We’ll help you understand that taking care of yourself after an accident isn’t being dramatic or overdoing it – it’s being smart. Because your future self will thank you for getting this right.
When Your Body Becomes a Crime Scene (And You’re Both Victim and Detective)
Here’s the thing about car accidents – your body doesn’t care if you were just grabbing coffee or heading to your kid’s soccer game. When metal meets metal at any speed above, well, zero, your body becomes this fascinating (and frankly annoying) case study in physics meets biology.
Think of it like this: you’re sitting in your car, minding your own business, when suddenly you’re part of an unwanted physics experiment. Your car stops – maybe gently, maybe not so much – but your body? It keeps going until something stops it. Usually the seatbelt, the airbag, or… yikes… parts of your car you never wanted to get acquainted with.
The Sneaky Truth About Adrenaline
Now here’s where it gets tricky, and honestly, kind of unfair. Right after an accident, your body floods itself with adrenaline – nature’s own little emergency cocktail. It’s like your internal systems just chugged three energy drinks and decided they’re invincible.
You might feel fine. Great, even. You’re walking around, talking to police officers, maybe even helping push cars out of traffic. Meanwhile, your body is basically running on biological duct tape and determination.
The problem? Adrenaline is a really convincing liar. It masks pain, reduces inflammation temporarily, and generally makes you feel like you could bench press your car. But here’s the catch – it wears off. Usually within a few hours, sometimes by the next morning, and that’s when the real party starts.
Why “I Feel Fine” Might Be Famous Last Words
This is probably the most counterintuitive thing about accident injuries: the absence of immediate pain doesn’t mean the absence of injury. It’s like your smoke detector going off after the fire department has already arrived – the warning system is a little behind the actual event.
Soft tissue injuries (we’re talking muscles, ligaments, tendons – basically all the squishy bits that hold you together) are particularly sneaky. They’re like that friend who seems totally fine at the party but texts you three days later saying they’re never drinking again.
Whiplash, for instance, often doesn’t announce itself until 24-48 hours later. Your neck basically got shaken like a maraca, but it takes time for the inflammation and stiffness to set in. Fun fact: even low-speed accidents (we’re talking 5-10 mph) can cause whiplash. Physics doesn’t really care about your speedometer reading.
The Domino Effect Nobody Warns You About
Here’s something they don’t mention in driver’s ed – injuries from car accidents are rarely neat and contained. Your body is this incredibly connected system, kind of like a really complex game of Jenga. Move one piece, and everything else has to compensate.
Let’s say you injured your lower back. Seems straightforward enough, right? But now you’re walking differently to avoid pain, which changes how your hips move, which affects your knees, which might even mess with your neck as your posture shifts. Before you know it, you’re dealing with issues that seem completely unrelated to where you initially hurt.
It’s like when you favor one leg after stubbing your toe, and three days later your opposite hip is killing you. Your body is constantly trying to protect the injured area, sometimes at the expense of everything else.
When “Wait and See” Becomes “Wait and Regret”
Insurance companies love the “wait and see” approach. And honestly, I get it – nobody wants to overreact to every minor fender bender. But here’s where it gets complicated…
Some injuries actually get worse without proper treatment. That minor muscle strain can turn into chronic tension patterns. What feels like a simple headache might be the beginning of post-concussion syndrome (yes, you can get a concussion even if you never hit your head directly – your brain basically becomes a marble rattling around in a jar).
The tricky part is that early treatment often prevents these minor issues from becoming major problems. It’s like fixing a small crack in your windshield before it spider-webs across the entire thing. Much easier, much cheaper, much less complicated when you catch it early.
And then there’s the whole legal side of things, which… well, that’s a whole other conversation. But let’s just say documentation matters, and waiting three weeks to seek treatment doesn’t exactly strengthen your case that you were actually injured.
Getting the Right Medical Care After Your Accident
Here’s the thing about car accident injuries – they’re sneaky little troublemakers. You might walk away feeling like Superman, only to wake up the next morning moving like the Tin Man before he got his oil can. That’s why you need to see a healthcare provider within 24-48 hours, even if you feel fine.
Don’t just waltz into any urgent care clinic, though. Look for providers who actually understand car accident injuries – orthopedic specialists, chiropractors with accident experience, or physical medicine doctors. They know the difference between “slept wrong” neck pain and whiplash that could haunt you for months.
Documenting Everything Like Your Settlement Depends On It
Because… well, it probably does. Take photos of everything – your car, the other car, the intersection, any visible injuries (even if they seem minor). But here’s what most people miss: document how you *feel* every single day.
Keep a pain journal. Sounds dramatic? Maybe. But when you’re sitting in a lawyer’s office six months later trying to remember if your headaches started immediately or three days after the accident, you’ll thank yourself. Note your pain levels, what activities hurt, how your sleep got disrupted. Your future self will worship you for this foresight.
Also – and this is crucial – keep every single medical receipt, every parking receipt from doctor visits, even receipts for ice packs or heating pads you bought. Insurance companies love to play detective with your expenses.
Working with Insurance Companies Without Getting Played
Insurance adjusters are trained to be friendly. They’ll call you quickly, maybe even the same day, sounding genuinely concerned about your wellbeing. Here’s your reality check: they work for the insurance company, not you. Their job is to minimize what their company pays out.
Be polite but careful. Don’t admit fault (even if you think you might have contributed – let the professionals sort that out). Don’t say you’re “fine” or “not hurt” – you might not know yet. A simple “I’m still being evaluated by medical professionals” works perfectly.
Get everything in writing. That verbal promise about covering your rental car? Meaningless unless it’s documented. And never – and I mean *never* – sign anything without having someone knowledgeable review it first.
Finding the Right Treatment Team
Your family doctor is wonderful for your annual physical, but car accident injuries need specialists who see this stuff daily. Start with your primary care doctor for initial evaluation, but don’t be surprised if they refer you out quickly.
Chiropractors, physical therapists, orthopedic doctors, pain management specialists – you might need a whole village. The key is finding providers who communicate well with each other and with insurance companies. Ask potential providers: “How often do you treat car accident patients?” and “Do you work with personal injury attorneys?” Their comfort level with these questions tells you everything.
When to Call a Personal Injury Attorney
Most people think they need a lawyer only if they’re catastrophically injured. Not true. Consider calling if any of these apply: the other driver was clearly at fault, you’re dealing with significant medical bills, you’re missing work, the insurance company is being difficult, or you’re just feeling overwhelmed by the process.
Many personal injury attorneys work on contingency – meaning they don’t get paid unless you do. Most offer free consultations, so you can get professional advice about whether your situation warrants legal representation. Think of it as getting a second opinion, but for your legal rights instead of your medical condition.
The Hidden Recovery Timeline Reality
Here’s what nobody tells you: car accident recovery rarely follows a neat timeline. You might feel better, then worse, then better again. Some days you’ll think you’re completely healed, others you’ll wonder if you’ll ever feel normal again.
This roller coaster is completely normal, but it’s also why you shouldn’t rush to settle with insurance companies. That “final” settlement is exactly that – final. Once you sign, there’s no going back if your symptoms return or worsen.
Most soft tissue injuries take 6-12 weeks to resolve, but everyone heals differently. Some people bounce back in a few weeks; others deal with lingering effects for months. Don’t let anyone – insurance adjusters, well-meaning friends, or even some medical providers – pressure you into believing you should be “over it” by now.
Give yourself permission to heal at your own pace. Your body went through trauma, even in a “minor” accident. Respect that process.
When Insurance Companies Play Hard to Get
Let’s be real – dealing with insurance after a car accident feels like speaking a foreign language while juggling flaming torches. You’re already hurting, probably stressed about your car, maybe missing work… and then you’ve got to become a claims adjuster overnight?
The biggest trap people fall into is accepting that first settlement offer. Insurance companies bank on you being overwhelmed and wanting this whole mess behind you. But here’s what most folks don’t realize: that initial offer is almost always their lowball starting point. They expect you to negotiate.
Your game plan? Document everything. I mean everything. Photos of your injuries (even if they seem minor), all your medical appointments, every prescription, even the Uber receipts when you couldn’t drive yourself. Create a folder – physical or digital – and dump it all in there. When the adjuster calls asking for records, you’ll have them ready instead of scrambling through three months of paperwork at 9 PM.
And don’t sign anything without understanding what you’re agreeing to. That innocent-looking medical release form? It might give them access to your entire medical history going back to your wisdom teeth removal in college.
The “I Feel Fine” Trap
This one gets people every single time. You walk away from the accident feeling okay – adrenaline’s a hell of a thing – and figure you dodged a bullet. Fast forward 48 hours, and you can barely turn your head.
The problem is, once you’ve told the insurance company you’re fine, it becomes much harder to get coverage for treatment later. They’ll pull that initial statement and use it against you faster than you can say whiplash.
Here’s what smart people do: get checked out anyway. Even if you feel fine. Even if you think it’s unnecessary. A quick visit to urgent care or your doctor creates a paper trail that says “Yes, I was in an accident, and yes, I got medical attention.” You’re not being dramatic – you’re being smart.
Finding the Right Doctor (Spoiler: It’s Harder Than It Should Be)
Not all doctors understand car accident injuries. Your family physician might be amazing at handling your annual physical, but soft tissue injuries from crashes? That’s specialized territory.
You need someone who understands the mechanics of car accidents, knows how to document injuries properly for legal and insurance purposes, and won’t rush you out the door after five minutes. This isn’t about finding someone to exaggerate your injuries – it’s about finding someone who takes them seriously.
Start by asking around – friends, family, even your lawyer if you have one. Look for clinics that specifically mention auto accident treatment. And don’t be afraid to ask potential doctors about their experience with car accident cases during your initial consultation.
The Settlement Timeline Reality Check
People always ask, “How long will this take?” as if there’s some universal timer counting down. The honest answer? It depends on way more factors than you’d think.
Minor injuries with clear medical records? Maybe a few months. But if you’re still treating, if there’s dispute about who was at fault, if multiple cars were involved… we could be talking a year or more. I’ve seen simple rear-end collisions drag on for 18 months because someone’s MRI showed something unexpected.
The key is not letting the timeline stress drive you to settle too quickly. Your medical treatment should guide the timeline, not insurance company pressure or your desire to “move on.” You can’t un-sign a settlement agreement.
Managing the Emotional Roller Coaster
Nobody talks about this part enough, but car accidents mess with your head in ways that have nothing to do with concussions. One day you’re confident and ready to fight for fair compensation… the next, you just want to take whatever they’re offering and be done with it.
This emotional whiplash is completely normal. You’re dealing with physical pain, financial stress, insurance bureaucracy, and probably some anxiety about driving. Of course you’re going to have ups and downs.
Find someone to talk to – whether that’s a counselor, a support group, or just a trusted friend who’ll listen without trying to “fix” everything. Sometimes you need to vent about the insurance adjuster who hasn’t returned your calls for two weeks, and that’s okay.
Remember: taking care of your emotional health isn’t separate from your physical recovery. They’re connected in ways we’re only beginning to understand.
What You Can Really Expect During Recovery
Let’s be honest here – everyone wants to know how long this is going to take. It’s human nature, right? You’re probably sitting there with a sore neck or aching back, wondering if you’ll ever feel normal again. And while I wish I could give you a neat little timeline tied up with a bow… recovery just doesn’t work that way.
Most people start feeling some relief within the first few weeks of treatment. Notice I said “some” relief – not complete, magical healing. Your body’s been through trauma, even if it seems minor. Those first two to four weeks? Think of them as your body’s way of saying “hold on, let me figure out what just happened here.”
Some folks bounce back surprisingly quickly. Others – and this doesn’t mean anything’s wrong with you – need several months to feel like themselves again. I’ve seen patients who were rear-ended at 15 mph take longer to heal than someone who walked away from a much more dramatic accident. Bodies are weird like that.
The thing is, healing isn’t linear. You might have three good days, then wake up feeling like you got hit by that car all over again. That’s… actually pretty normal. Frustrating? Absolutely. But normal.
Your Treatment Plan Will Evolve
Here’s what typically happens: you’ll start with more frequent appointments – maybe two or three times a week. Your chiropractor or physical therapist needs to see how your body responds to treatment, and honestly, those first few sessions are as much diagnostic as they are therapeutic.
After a few weeks, assuming things are moving in the right direction, you’ll probably space out your visits. Maybe down to twice a week, then once a week. Some people graduate to maintenance visits – you know, that monthly tune-up that keeps everything running smoothly.
But here’s the thing that catches people off guard… sometimes your treatment plan needs to pivot. Maybe that neck pain clears up beautifully, but now your lower back is acting up because you’ve been compensating. Or perhaps you’re doing great with chiropractic care, but your doctor thinks some physical therapy would speed things along.
Don’t panic if this happens. It’s not a sign that something’s going wrong – it’s actually a sign that your healthcare team is paying attention and adjusting as needed.
The Mental Game Nobody Talks About
Can we talk about something for a minute? The emotional stuff. Because nobody really prepares you for how a car accident messes with your head, even when your injuries seem “minor.”
You might find yourself tensing up every time you drive past the intersection where it happened. Or maybe you’re just… tired all the time. Not sleepy-tired, but that bone-deep exhaustion that comes from your body working overtime to heal itself. Some people feel anxious or irritable – and then feel guilty about feeling that way because “it wasn’t even that bad.”
This is all part of it. Your nervous system got rattled along with everything else, and it takes time to settle back down. If these feelings stick around or get worse, definitely mention it to your doctor. There’s no shame in needing some extra support.
Planning for the Long Game
Most car accident injuries resolve within three to six months with proper treatment. But – and this is important – “resolved” might not mean “exactly like before.” Some people discover they need to be more mindful about their posture, or that they benefit from regular exercise they never did before.
Think of it less like returning to factory settings and more like… upgrading your maintenance routine. Maybe you’ll learn stretches that actually help you feel better than you did before the accident. Or perhaps you’ll finally address that old sports injury that’s been lurking in the background.
The key is staying engaged with your treatment and communicating with your team. If something’s not working, speak up. If you’re feeling discouraged, say so. If you’re having a great week, celebrate that too.
Recovery isn’t just about getting back to where you were – sometimes it’s about getting to where you want to be. And that? That might just be the silver lining you didn’t know you were looking for.
You know what? After going through all these questions, I hope you’re feeling a bit more grounded about what to expect if you’re dealing with car accident injuries. It’s completely normal to feel overwhelmed – your body’s been through something traumatic, and honestly, the whole process can feel like you’re navigating a maze blindfolded.
But here’s the thing that I really want you to remember… you don’t have to figure this out alone. Whether you’re dealing with lingering pain that just won’t quit, insurance companies that seem to speak in riddles, or that nagging worry that maybe you should have gotten checked out sooner (we’ve all been there), there are people who genuinely want to help you feel better.
You’re Not Being Dramatic
I can’t tell you how many people I’ve talked to who downplay their symptoms or feel guilty for seeking treatment weeks after their accident. “Maybe it’s all in my head,” they’ll say. Or “I should just tough it out.”
Stop right there. Your pain is real. Your discomfort matters. And getting the care you need isn’t being weak – it’s being smart.
The truth is, your body has an incredible way of compensating when something’s not quite right. You might not even realize how much you’ve been favoring one side, or how those tension headaches have become your new normal. Sometimes it takes a professional eye to spot what’s really going on and help you get back to feeling like yourself again.
Moving Forward (Really Moving Forward)
Recovery isn’t always a straight line – and that’s perfectly okay. Some days you’ll feel great, others… not so much. That’s your body’s way of healing, and it’s completely normal. What matters is that you’re not suffering in silence or letting things slide because you think they’ll just go away on their own.
Whether you’re dealing with whiplash that’s making work miserable, back pain that’s affecting your sleep, or just that general feeling that something’s “off” since your accident – these things have a way of improving dramatically with the right care. And yes, that includes addressing any weight changes that might have happened since your mobility took a hit.
Here’s What I’d Love for You to Do
If any of this resonates with you, would you consider reaching out? Not because you have to, but because you deserve to feel better. Our team understands that every accident is different, every person heals differently, and every situation comes with its own set of concerns.
We’re not here to pressure you or make promises we can’t keep. We’re here to listen, to answer your specific questions (the ones that Google can’t quite address), and to work with you on a plan that actually makes sense for your life.
Give us a call when you’re ready – whether that’s today, next week, or when you finally decide you’re tired of dealing with that persistent ache. We’ll be here, and we’ll figure it out together. Because honestly? You’ve been through enough already. Let us help you feel like yourself again.